Injuries to the spinal cord can be life-altering, with effects ranging from mild sensory changes to complete paralysis. For clinicians, patients, and caregivers alike, understanding what a spinal cord injury (SCI) is—and how it affects the body—is essential to optimizing recovery and guiding care.
Spinal cord injuries not only disrupt movement and sensation but can profoundly affect autonomic regulation, posture, balance, and overall brain-body communication. This post provides a clear overview of spinal cord anatomy, the types and consequences of SCI, and how neurorehabilitation strategies—including those informed by chiropractic neurology—can play a role in restoring function.
A Brief Overview of Spinal Cord Anatomy and Physiology
The spinal cord is a cylindrical bundle of nerve tissue encased within the vertebral column, extending from the brainstem (at the level of the medulla oblongata) to approximately the L1–L2 vertebral level in adults. It serves as the main communication highway between the brain and the rest of the body.
Structural Divisions
The spinal cord is divided into four main regions:
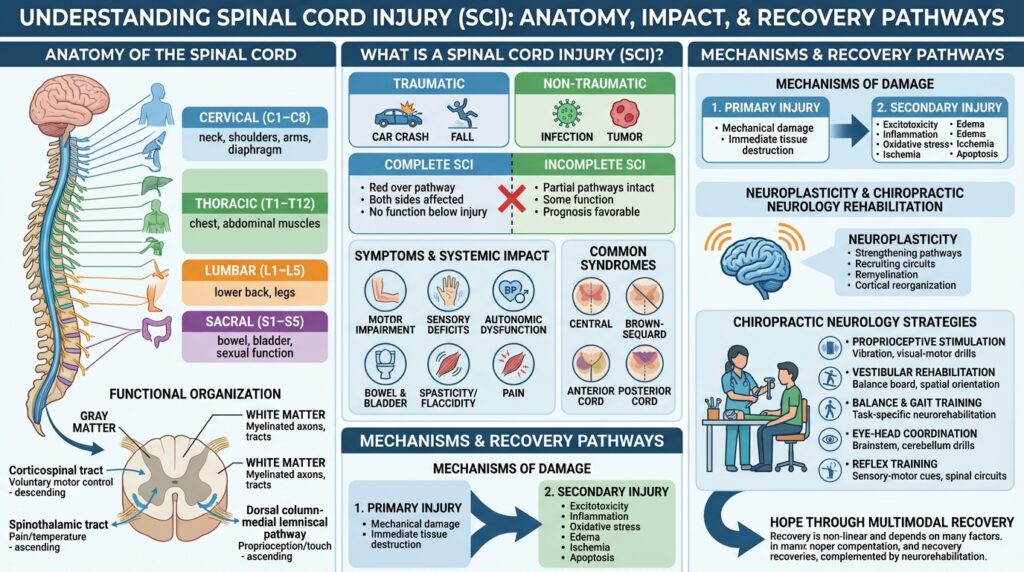
- Cervical (C1–C8) – controls the neck, shoulders, arms, and diaphragm
- Thoracic (T1–T12) – innervates the chest and abdominal muscles
- Lumbar (L1–L5) – serves the lower back and legs
- Sacral (S1–S5) – contributes to bowel, bladder, and sexual function
Each segment of the spinal cord gives rise to a pair of spinal nerves, which exit through the intervertebral foramina to serve specific body regions (dermatomes and myotomes).
Functional Organization
The spinal cord consists of:
- Gray matter (center): Contains neuronal cell bodies, including motor neurons in the anterior (ventral) horn and sensory interneurons in the posterior (dorsal) horn.
- White matter (outer): Contains myelinated axons forming ascending tracts (carrying sensory input to the brain) and descending tracts (carrying motor commands from the brain).
Key tracts include:
- Corticospinal tract – voluntary motor control
- Spinothalamic tract – pain and temperature sensation
- Dorsal column-medial lemniscal pathway – proprioception, vibration, and fine touch
Understanding this basic anatomy is crucial because the location and severity of an injury dictate the specific deficits a person may experience.
What Is a Spinal Cord Injury?
 A spinal cord injury is defined as any damage to the spinal cord that results in temporary or permanent changes in its function. Injuries can be traumatic (e.g., from motor vehicle accidents, falls, or violence) or non-traumatic (due to infection, tumor, degenerative disease, or ischemia).
A spinal cord injury is defined as any damage to the spinal cord that results in temporary or permanent changes in its function. Injuries can be traumatic (e.g., from motor vehicle accidents, falls, or violence) or non-traumatic (due to infection, tumor, degenerative disease, or ischemia).
Types of SCI
- Complete SCI
– No voluntary movement or sensory function remains below the level of injury
– Both sides of the body are equally affected
– Indicates total disruption of neural pathways - Incomplete SCI
– Some function remains below the level of injury (e.g., partial sensation or movement)
– May affect one side of the body more than the other
– Prognosis is generally more favorable
Common Syndromes
- Central Cord Syndrome – typically affects the cervical spine; more motor impairment in upper limbs than lower limbs
- Brown-Séquard Syndrome – hemisection of the spinal cord; causes ipsilateral motor loss and contralateral pain/temperature loss
- Anterior Cord Syndrome – damage to the anterior two-thirds of the spinal cord; loss of motor function, pain, and temperature sensation
- Posterior Cord Syndrome – rare; loss of proprioception and fine touch below injury
Symptoms and Systemic Impact
The effects of SCI depend on the level and completeness of the injury. Common symptoms include:
- Motor impairment – weakness or paralysis
- Sensory deficits – numbness, tingling, or loss of proprioception
- Autonomic dysfunction – blood pressure instability, thermoregulation issues, sexual dysfunction
- Bowel and bladder dysfunction
- Spasticity or flaccidity – altered muscle tone due to loss of upper or lower motor neuron input
- Pain – neuropathic pain is common after SCI and can be difficult to manage
Even injuries that leave the spinal cord anatomically intact can cause significant dysfunction if they interfere with neurotransmission or inflammation.
Mechanisms of Damage
SCI evolves through two phases:
1. Primary Injury
This refers to the initial mechanical damage from trauma—compression, laceration, or transection. It causes immediate destruction of neural tissue, vascular damage, and disruption of axonal pathways.
2. Secondary Injury
This occurs minutes to days after the primary insult and involves:
- Excitotoxicity (excessive glutamate)
- Inflammation and immune response
- Oxidative stress and free radical formation
- Edema and ischemia
- Demyelination and apoptosis
Secondary injury often worsens the original damage, making early management and neuroprotection critical.
Neuroplasticity and the Potential for Recovery
Historically, spinal cord injuries were seen as irreversible. However, contemporary research highlights the plasticity of the nervous system—its ability to reorganize, remap, and regenerate to some extent, particularly in incomplete injuries.
Neuroplasticity is the foundation of modern SCI rehabilitation. It involves:
- Strengthening existing pathways
- Recruiting adjacent or redundant circuits
- Encouraging remyelination
- Promoting cortical reorganization
Rehabilitative efforts must be task-specific, repetitive, and multisensory to effectively harness this adaptive potential.
The Role of Chiropractic Neurology in SCI Rehabilitation
Chiropractic neurology applies the principles of functional neuroanatomy and neuroplasticity to assess and enhance nervous system function. For patients with spinal cord injuries—particularly incomplete SCIs—this approach can provide targeted, non-invasive interventions that support central integration, coordination, and function.
Rather than focusing solely on motor output, chiropractic neurologists address sensorimotor loops, reflex integrity, balance, coordination, and vestibular function. These systems often become disorganized after spinal injury but can be retrained with appropriate input.
Examples of Chiropractic Neurology Strategies for SCI Include:
- Proprioceptive stimulation using joint positioning exercises, vibration, or visual-motor coordination drills
- Vestibular rehabilitation to improve postural control and spatial orientation
- Balance and gait training using task-specific neurorehabilitation methods
- Eye-head coordination drills to facilitate brainstem and cerebellar involvement
- Reflex training to engage spinal circuits through predictable sensory-motor cues
All interventions are grounded in neurological specificity, meaning they target known pathways and circuits based on the patient’s presentation.
Looking Ahead: Hope Through Multimodal Recovery
Although SCI remains a serious and often life-changing condition, advances in neurorehabilitation are providing new pathways to functional improvement. Recovery is rarely linear and depends on many factors, including injury type, timing of intervention, and intensity of therapy.
Chiropractic neurology offers a neuroscience-based, non-invasive framework for optimizing recovery by stimulating neuroplastic mechanisms across sensory, motor, and integrative systems. While not a replacement for acute medical care or surgical intervention, this approach complements conventional therapy and provides a valuable toolset for chronic-phase recovery and functional enhancement.
If you or someone you love is suffering from a spinal cord injury and you would like to learn how chiropractic neurology can help, contact the team at Georgia Chiropractic Neurology Center today. We look forward to hearing from you.
Written by Sophie Hose, DC, MS, DACNB, CCSP
Peer-Reviewed References
- Behrman, A. L., Ardolino, E. M., & Harkema, S. J. (2017). Activity-based therapy: From basic science to clinical application for recovery after spinal cord injury. Journal of Neurologic Physical Therapy, 41(Suppl 3), S39–S45.
— Outlines principles of neuroplasticity and task-specific rehabilitation in SCI. - Courtine, G., & Sofroniew, M. V. (2019). Spinal cord repair: Advances in biology and technology. Nature Medicine, 25(6), 898–908.
— A cutting-edge review of experimental and clinical approaches to spinal cord repair. - Kakulas, B. A. (1999). The applied neuropathology of human spinal cord injury. Spinal Cord, 37(2), 79–88.
— Reviews the pathological basis of SCI and implications for recovery. - Raineteau, O., & Schwab, M. E. (2001). Plasticity of motor systems after incomplete spinal cord injury. Nature Reviews Neuroscience, 2(4), 263–273.
— Highlights mechanisms of plasticity in descending motor systems post-injury. - Zehr, E. P. (2006). Training-induced plasticity in human spinal cord function. Journal of Applied Physiology, 101(6), 1785–1794. — Discusses spinal reflex modulation and its application to rehabilitation.
